Understanding The Impact Of Microbiome On Mental Health
The mutualistic symbiosis between the gastrointestinal microbiota and the cerebral cortex has ascended to an unparalleled echelon of scholarly interest in recent years. Intellectual luminaries have meticulously delineated that the impact of microbiome on mental health is far more labyrinthine than previously conjectured. The gut microbiome, an immense consortium teeming with trillions of commensal, symbiotic, and pathogenic microorganisms, wields a prodigious influence over holistic physiological and psychological homeostasis, encapsulating mental health.
The mutualistic symbiosis between the gastrointestinal microbiota and the cerebral cortex has ascended to unparalleled scholarly interest in recent years. Intellectual luminaries have meticulously delineated that the impact of microbiome on mental health is far more labyrinthine than previously conjectured. The gut microbiome, an immense consortium teeming with trillions of commensal, symbiotic, and pathogenic microorganisms, wields a prodigious influence over holistic physiological and psychological homeostasis, encapsulating mental health.
How Microbiome Affects Mental Health
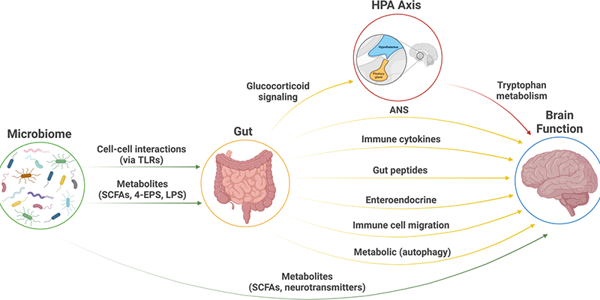
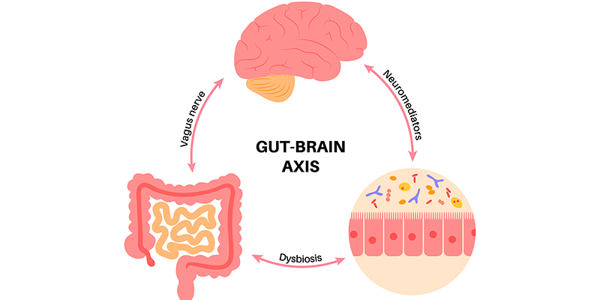
The gut microbiome interfaces with the encephalon through the gut-brain axis, an intricate conglomeration of neural, endocrine, and immunological channels. This elaborate symbiotic interplay elucidates how the microbiome affects mental health. For instance, specific bacterial taxa within the gut microbiome biosynthesize neuroactive compounds, including serotonin and dopamine, which are paramount in modulating affective states and cognitive functions. Perturbations within this macrobiotic milieu can precipitate a cascade of dysregulation in neurotransmitter pathways, thereby disrupting mental equilibrium.
Determinants Influencing Microbiome And Mental Health
A myriad of exogenous and endogenous variables can modulate the impact of microbiome on mental health, including dietary practices, chronic psychosocial stressors, and pharmacotherapeutic agents. A diet replete with nutritionally devoid, processed alimentary substances and lacking dietary fibre can instigate a dysbiotic shift within the gut microbiome. This state has been concomitantly associated with a spectrum of neuropsychiatric disorders, such as generalized anxiety disorder and major depressive disorder. Additionally, chronic stress is a potent etiological factor capable of inducing deleterious alterations in the gut microbiome, further exemplifying the microbiome's role in mental wellness.
- Diet: Nutritional inadequacies engender dysbiosis, thereby compromising mental health.
- Stress: Persistent stressors elicit perturbations within the gut microbiome, exacerbating neuropsychiatric symptoms.
- Medications: Specific pharmacological interventions, particularly broad-spectrum antibiotics, deleteriously influence the gut microbiome.
Microbiome’s Role In Mental Wellness
Many empirical inquiries have substantiated the microbiome's role in mental wellness. They have unveiled a robust correlation between gut microbiota homeostasis and psychological well-being. For example, probiotics—beneficial commensal microorganisms—have demonstrated therapeutic efficacy in ameliorating the symptomatic manifestations of mood disorders, including depression and anxiety. This underscores the pivotal notion that maintaining a robust and diverse gut microbiome is quintessential for preserving mental wellness.
Challenges In Research And Treatment
While the microbiome's role in mental wellness holds immense potential, it has significant epistemological and methodological challenges. The gut microbiome constitutes an extraordinarily complex and dynamic ecosystem, with substantial interindividual variability that complicates the development of universalized therapeutic paradigms. Moreover, the precise mechanistic pathways through which the microbiome's impact on mental health materializes remain obfuscated, posing a formidable obstacle to formulating targeted interventions.
The Evolution Of Microbiome Research In Mental Health
The inquiry into the impact of microbiome on mental health has experienced a profound metamorphosis over recent epochs. Initially relegated to the fringes of scientific dogma, microbiome research has ascended to prominence within psychiatry and neurobiology. Cutting-edge metagenomic sequencing methodologies have unveiled specific microbial clades implicated in mental health, disclosing intricate paradigms that eluded prior detection.
Pivotal Milestones In Microbiome Research
- Human Microbiome Project (HMP): This seminal initiative established the first exhaustive cartography of the human microbiome, yielding unprecedented insights into how microbiome affects mental health.
Psychobiotics: The discernment of psychobiotics—microorganisms with the potential to modulate central nervous system activity—has revolutionized our comprehension of the microbiome's role in mental wellness.
- Microbiota-Gut-Brain Axis Models: The advent of sophisticated in vivo and in vitro simulacra has deepened our understanding of the bidirectional crosstalk between the gut and the brain, illuminating novel dimensions of the microbiome's impact on mental health.
Unveiling The Microbial Signatures Of Psychiatric Disorders
Emergent data posits that discrete microbial signatures may be concurrent with distinct psychiatric pathologies. Through meticulous analysis of gut microbiota composition in individuals with conditions such as depression, schizophrenia, and bipolar disorder, researchers have uncovered singular microbial topographies that may function as diagnostic biomarkers.
Microbial Dysbiosis And Psychiatric Pathogenesis
- Depression: A conspicuous diminution in microbial diversity, particularly in the prevalence of Bifidobacterium and Lactobacillus species, has been correlated with depressive symptomatology, underscoring how the microbiome affects mental health.
- Schizophrenia: Perturbations in gut microbiota composition, exemplified by a decline in Firmicutes and a proliferation of Proteobacteria, have been implicated in the pathogenesis of schizophrenia, highlighting the impact of microbiome on mental health.
- Bipolar Disorder: Novel investigations suggest that individuals with bipolar disorder exhibit idiosyncratic gut microbiome profiles, potentially contributing to the cyclicality of mood disturbances, thereby affirming the microbiome’s role in mental wellness.
Microbiome Modulation As A Therapeutic Modality
As the elucidation of how the microbiome affects mental health advances, there is burgeoning interest in exploring microbiome modulation as a feasible therapeutic modality for psychiatric ailments. This approach entails intentionally altering gut microbiota composition to reestablish eubiotics and alleviate mental health symptoms.
Pioneering Microbiome-Based Therapies
Prebiotics are indigestible alimentary constituents that selectively stimulate the proliferation of beneficial gut bacteria, proffering a novel stratagem to enhance the microbiome's role in mental wellness.
- Synbiotics: A synergistic amalgamation of probiotics and prebiotics engineered to optimize the therapeutic efficacy of gut microbiota modulation, manifesting a considerable microbiome impact on mental health.
- Nutraceuticals: Bioactive constituents derived from dietary sources that benefit gut microbiota, presenting a promising vector for preventing and managing psychiatric disorders through targeted modulation of the gut-brain axis.
The Ethical Quandaries Of Microbiome Research
The rapid proliferation of microbiome research, particularly in how microbiome affects mental health, has engendered a host of ethical quandaries. As researchers continue to decipher the complexities of the gut-brain axis, it is imperative to contemplate the moral ramifications of manipulating the human microbiome, especially within vulnerable populations afflicted with mental health disorders.
Salient Ethical Conundrums
Informed Consent: Ensuring participants possess comprehensive cognizance of microbiome-based interventions' potential perils and benefits, particularly given this discipline's embryonic stage.
- Privacy and Data Security: Safeguarding the sensitive health data gleaned from microbiome sequencing could be exploited to predict an individual's susceptibility to mental health disorders.
Future Directions
Notwithstanding these formidable challenges, the inquiry into how the microbiome affects mental health continues to advance rapidly. Future research endeavours are anticipated to focus on elucidating and characterizing specific bacterial strains that confer the most pronounced benefits for mental health. This could pave the way for precision microbiome-based therapies, wherein individuals receive bespoke probiotic regimens or nutraceutical prescriptions tailored to their distinctive gut microbiome profiles.
- Precision Medicine: Custom-tailored therapeutic regimens predicated on individual microbiome profiles.
- Strain-Specific Inquiry: Identifying and isolating bacterial strains with the most significant psychobiotic potential.
Conclusion
The microbiome's ramifications on neuropsychological equanimity augur an esoteric paradigm shift in the ontological and pragmatic frameworks of neuropsychiatric disorder management. As scientific discourse progressively elucidates the cryptic and labyrinthine intricacies of the gut-brain symbiosis, it becomes incontrovertibly axiomatic that the microbiome's influence on neurocognitive homeostasis is irreplaceable.